
At the same time nursing schools can't raise their enrollments, complaints about stressful working conditions, too much overtime and low pay have spurred many nurses to leave the profession altogether. (According to Nursing Professor David Keepnews, nearly 20 percent of licensed registered nurses are not practicing.) "Seeing nurses as angels of mercy has got to go," retired Nursing Professor Jim Bush flatly states. "That's nice, but you can't raise a family on that."
Lack of funding is what has put nursing schools like the UW in a bind. The UW simply doesn't have the money to hire enough clinical faculty, who provide essential hands-on training for students outside of the classroom. At the school's Seattle campus, for example, the size of the faculty has decreased by 25 percent since 1978, while there has been no such decline in the number of students.
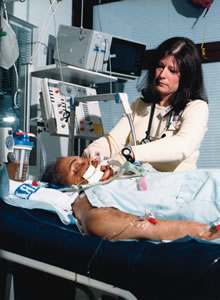
UW Medical Center Nurse Victoria Hutman, '99, examines a patient. Photo by Gavin Sisk.
"We had to become entrepreneurial," explains Nursing Dean Nancy Fugate Woods. "We just don't have the resources we need." And with each faculty member only able to accommodate a maximum of eight students because of the hands-on nature of the job, that can add up to a lot of money.
So UW nursing officials asked area hospitals to shift some their recruitment budget away from newspaper ads and career fairs to pay the salary of a clinical instructor. This instructor would come from their nursing staff and work at the UW. Nursing students would work with that instructor for a year, then spend a designated amount of time working at the hospital.
Hospitals loved the idea because it was a way they could reward their best nurses with a sabbatical from the rigors of daily patient care. It also gave the hospitals a pipeline to prospective employees. And for the UW, it was a way to sustain enrollment without having to spend money it didn't have to hire additional faculty members.
"We have been trying to meet the increasing needs of the nursing labor force at a time when money for higher education is shrinking," adds Dean Woods. "We have been forced to do more with less, and this is one creative way to have more faculty without paying for it."
But finding clinical instructors isn't that easy. Teaching doesn't pay very well, benefits are not always provided, and the responsibilities are immense. And while hospitals want to get more nurses into the workplace, having nursing students on the floor increases the workloads of other nurses. And so it goes.
Another strategy has been having local hospitals offer loans to UW nursing students. In exchange, each student receiving such funding would repay the loan by working at the hospital. The idea, hatched by the Veteran's Affairs Department, allowed nine UW bachelor of nursing students to get full tuition support and a stipend in exchange for their agreement to work in a veteran's hospital for two years after graduation. UW Medical Center, Harborview and Virginia Mason Medical Center began similar programs during the past two years. And there is a good chance other Seattle-area hospitals, such as Northwest and Evergreen, might join as well.
Another idea for getting students in the door is an accelerated baccalaureate program. Under this idea, about 20 students in a class of 80 would complete their schooling in five consecutive quarters instead of the usual six quarters with summers off.
But simply pushing more students through nursing programs isn't the only answer, according to Bush, the retired nursing professor. "You need seasoned, mature faculty teaching," he explains. "You don't want to pump through students who aren't prepared. You can't just focus on numbers of people. Quality is still the main issue." And quality can be threatened. Bush recalls the time he recently went to have his blood pressure checked and the nurse tending him didn't use the correct sized cuff, creating an inaccurate reading.