
by Julie Garner
Dellinger takes an unusual tact when he meets his obese patients for the first counseling session-he tries to talk them out of the procedure. Because they are so eager to solve the problem, they don't have a realistic view of the risk, he says.
Although the methods of performing bariatric surgery vary somewhat, all stomach surgery is major and carries risk. Fifteen to 20 percent of bariatric surgery patients develop complications, 10 percent develop a wound infection, and 15 to 20 percent experience psychological problems such as depression.
The official U.S. death rate is 0.5 percent or about 1 out of 300 surgeries. However, Dellinger says the death rate in Washington state is 2 percent or about 1 out of 50 surgeries. He believes that's a more realistic national percentage as well.
Because of the risk, bariatric surgery is not a choice for the faint of heart. "Bariatric surgery is behavior modification with a hammer," says David Flum, assistant professor in the UW Department of Surgery and principal investigator for the research project.

Not everyone with a weight problem qualifies for bariatric surgery. Only adults who are "morbidly obese"-more than 100 pounds overweight-are eligible.
Another way to understand obesity is to look at a patient's Body Mass Index (BMI), which assesses your weight compared to your height. If you are 5 feet 8 inches with a weight of 150 pounds, you have a 22.8 BMI. A healthy adult BMI generally falls between 18.5 and 25.
If your BMI is more than 25, you are probably overweight. If it is 30 or higher, you are considered obese, and 40 or higher, you are "morbidly" or "super obese" and a candidate for surgery. Douglas had a 41.7 BMI prior to her surgery.
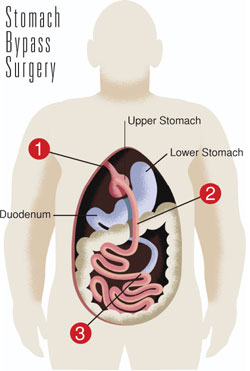
In a gastric bypass, the surgeon divides the stomach into a smaller upper section and a larger bottom section using staples that are similar to stitches. The top section of the stomach (called "the pouch") continues to hold food. After the stomach is divided, the surgeon connects a section of the small intestine to the pouch so that the food bypasses the rest of the stomach.
Gastric bypass surgery can now be done with a laparascope, a slender, illuminated optical or fiber-optic instrument that functions like a camera when it is inserted through an incision in the abdominal wall. The surgeon watches through a lens and video monitor. A laparascopic procedure is less invasive and allows for smaller incisions, a lower risk of large scars and hernias and a quicker recovery. This is the reason behind the skyrocketing number of bariatric surgeries in the U.S. However, this technique may not be available to the super obese because the large amount of fat and tissue prevents the use of a tiny instrument and smaller incisions.
Douglas resorted to this radical surgery because, after her initial dieting success, she couldn't maintain her ideal weight. Everyone who has ever gone on a diet knows that weight loss is hard, but keeping the pounds off is where the battle is really won or lost. "Ninety-five percent of the people who lose 5 to 10 percent of their body weight don't keep it off. Why are they so incapable? What else is there?" asks Flum.

The answer doesn't lie in poor character or lack of personal discipline, according to Flum. He and his colleagues already know that there are chemicals in the body that are designed to help keep weight on. Flum theorizes that there are good evolutionary reasons for the human body to resist weight loss. Over the centuries, people who survived famine were those who were most efficient at storing body fat, so natural selection favored this body type.
"When you lose weight by dieting, every signal in your body tells you to bring in more calories. Your body is essentially working against you when you lose weight. Is obesity the product of sloth or disease? That debate may be irrelevant. What underlies that debate is that there is a complex system in our bodies to help put the weight on and keep it on," says Flum.
By studying bariatric surgery patients, Flum and his colleagues hope to learn more about how the body's chemicals suppress or stimulate appetite. While the size of the "new" stomach made in gastric bypass surgery is vital in reducing the calories consumed, Flum and his colleagues believe that body chemicals, called peptides, also play a big role in successful weight loss and maintenance.
Even when stomach surgery is not tied to weight loss-such as surgery due to stomach cancer-doctors still find it results in a profound lack of appetite. "These patients aren't hungry. You'd expect they would be really hungry. This is the most intriguing aspect of bariatric surgery. If we can understand what makes people hungry and what takes hunger away in people who have gastric surgery, maybe we can find a nonsurgical solution to obesity," Flum says.
It's a strange twist of science that the quest for the ultimate diet pill might start with stomach surgery. Researchers speculate that gastric surgery, which bypasses most of the stomach and the duodenum (the first, shortest, and widest part of the small intestine), interferes or suppresses the production of ghrelin, a hormone that increases food intake in humans.
Go To: Page 1 | Page 2 | Page 3
Sidebar: Patch Work: Stomach Bypass Pioneer Dr. "Patch" Dellinger